
Clinical News
Topic: "Clarity Market" – Thailand’s Vision Bazaar.
By Dr. Loft
Date: May 11, 2025
Original Thai Version : https://www.loftoptometry.com/ตลาดชัดแห่งประเทศไทย
"Clarity Market"
The Clarity Market is a marketplace where the primary product is "selling clarity." It offers a variety of products ranging from high-safety standards to dangerously substandard goods. Regardless of the quality, every vendor competes for attention when the market opens, often resorting to embellishments, grandiose claims, and impressive marketing tactics to add perceived value to their clarity-related products. Some claims are true, some exaggerated, and some entirely false. However, in the Materialistic Economy, where resources are limited and the value of the "Clarity Market" is enormous, ethics often take a backseat.
Clarity itself has created a vast market because it is something everyone desires. No one can deny their need for clarity. This demand has driven continuous advancements in technology and innovation—ranging from display screens that evolved from CRT to flat-screen, LED, OLED, 4K, 5K, and even 8K retina displays. Movies and cameras today keep achieving higher levels of sharpness. The question is, how many hundreds of millions of pixels will be enough? The truth is, clarity is fundamentally important to people.
Because everyone wants to see clearly, they turn to the Clarity Market, which operates through various platforms—physical booths, stalls, rooms, buildings, online stores, Facebook, Shopee, Lazada, and other networks. These platforms provide clarity services based on each individual’s knowledge, experience, and financial capability. When the product is the same, the competition lies in attracting attention. Vendors amplify their voices; if truth alone isn’t engaging enough, they tweak it—presenting only half-truths to capture interest. The core message often boils down to: "My store offers clearer and better value."
The True Nature of Clarity
Genuine clarity is not easily achieved. It is the result of an integration of art and science, developed through knowledge, experience, and expertise. Helping patients "see the true essence of clarity" is not as simple as casual shoppers in the market might think. Because clarity seems easy to attain, many become victims of the market, ending up fearful, disillusioned, and avoiding the Clarity Market altogether.
Fortunately, in the era of 4G and 5G, people no longer have to visit the market physically. They can browse and compare all stores from home, reducing trial-and-error risks. As a result, fraudulent or exaggerated clarity providers will struggle to survive, while authentic providers will endure. Over time, over-the-top marketing gimmicks and misleading advertisements will fade away.
Do We Truly Understand Clarity?
A bigger issue is whether people truly understand the clarity they seek. Many chase after clarity without knowing its actual definition. In clinical optometry, clarity has specific standards and criteria, but the Thai Clarity Market remains chaotic because many vendors do not distinguish between proper and improper clarity. Without clear regulations, everyone operates in their own way.
A Standard That Has Never Been Established
In Thailand, there has never been an official standard for vision correction. There is no defined guideline on what constitutes a correct or incorrect eye examination. As a result, optical service quality varies drastically—from exceptionally high standards to businesses that focus solely on closing sales with no concern for accuracy.
One reason for this lack of standardization is that clinical optometry (Optometry Clinic) is still relatively new in Thailand. While the field has been established in the U.S. for over 124 years (since 1896), Thailand only introduced optometry education 18 years ago (2002) and officially recognized it as an academic faculty a few years ago.
Due to high tuition fees, lengthy study durations, and a shortage of educators, optometry programs are difficult to establish in universities. Over the past 20 years, Thailand has produced only about 300 licensed optometrists, which is extremely low compared to the country’s population. This explains why comprehensive vision assessment and binocular function testing—beyond simple eyeglass prescriptions—remain unstandardized in Thailand. Implementing a new standard would inconvenience older generations of optical professionals who operate without formal optometric training.
Consequences of a Lack of Standards
Without standards or regulations, eye care providers operate based on personal discretion, relying on their own ethical codes, which vary from person to person. Some professionals are highly ethical, while others are not. Since incorrect vision prescriptions do not immediately cause blindness or death, authorities rarely intervene. The belief that "wearing the wrong glasses never killed anyone" allows subpar practices to persist.
However, if research were conducted on car accidents and the visual impairments of drivers, shocking correlations might be found. Many traffic incidents attributed to "poor visibility" could stem from unaddressed personal vision problems. But in the absence of regulations, such issues are dismissed as mere bad luck.
Ignorance: The Root of Suffering
Ignorance is dangerous. A child who does not know that fire burns will put their hand in a flame. A child unaware of the dangers of playing with lighters might burn down a house. A child who does not understand guns can accidentally shoot someone. Similarly, adults who ignore the dangers of poor vision continue reckless habits—leading to consequences they fail to anticipate.
In the Clarity Market, "not knowing" or "not fully understanding" results in a lack of wisdom to foresee the consequences. When people do not know any better, they act carelessly, which affects patients—sometimes immediately, sometimes years later when it’s too late to fix the damage.
"Testing Until It Looks Sharp" – A Flawed Approach
In Thailand, many eye examinations rely on the flawed principle of "testing until it looks sharp." This means practitioners keep adjusting the prescription (add minus) until the patient says "it looks sharp", assuming that the final number is the correct one. However, clarity alone does not indicate correctness—it merely means the person can see as well as the average normal-sighted person. Whether their visual system is functioning properly is another matter entirely.
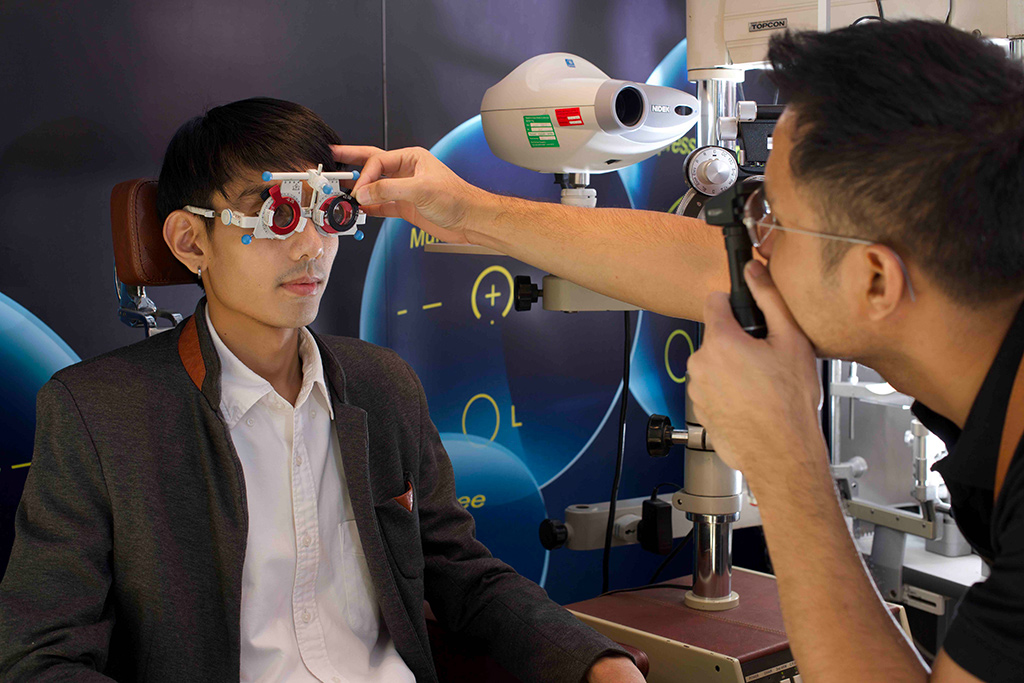
this sample image show truely comprehensive eye exam in optometry clinic , not just sell glasses.
Teachers always emphasize that "clear vision does not necessarily mean good binocular vision, and optometry is about enhancing vision and binocular vision, not just how seeing." The goal is to maximize the efficiency of visual function, both in terms of clarity and coordination between both eyes, rather than just achieving clear sight.
What Defines Correct Clarity?
Correct clarity occurs when light is focused into a single point that lands precisely on the retinal focal point while the eye's lens remains in a relaxed state. In other words:
SINGLE FOCAL POINT SHARP IMAGE FOCUS ON the FOVEA on the RETINA, WHILE ACCOMMODATION is RELAXED.
How Is This Achieved?
Blurred vision occurs when the focal point is not concentrated into a single spot but rather forms a focal line, commonly found in astigmatism, resulting in shadowed or doubled images. Alternatively, it can result from a single focal point that does not land precisely on the retina, leading to uniform blurriness across all axes—such as in nearsightedness or farsightedness without astigmatism. In myopia, the focal point falls in front of the retina, while in hyperopia, it falls behind the retina. Both conditions can also occur together.
Types of Refractive Errors Based on Focal Point Position:
- Simple Myopia – The focal point is concentrated but falls before the retina.
- Simple Hyperopia – The focal point is concentrated but falls behind the retina.
- Simple Myopic Astigmatism – One focal line is on the retina, the other falls in front.
- Simple Hyperopic Astigmatism – One focal line is on the retina, the other falls behind.
- Compound Myopic Astigmatism – Both focal lines fall before the retina.
- Compound Hyperopic Astigmatism – Both focal lines fall behind the retina.
- Mixed Astigmatism – One focal line falls before the retina, while the other falls behind.
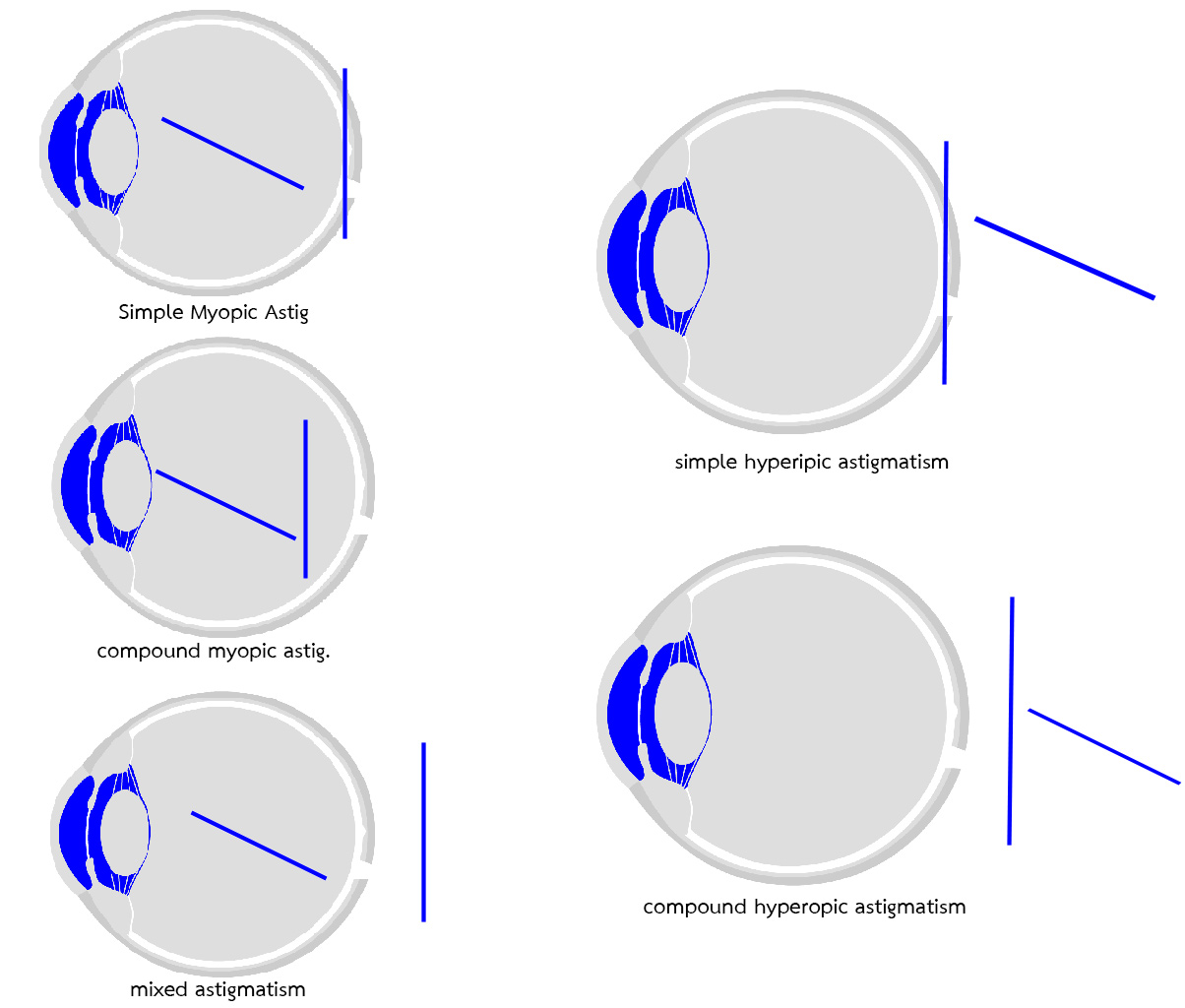
This image show how the focal line in difference visual problem align on the retina.
To achieve correct clarity, the focal lines must be converted into a single focal point, which then must be positioned precisely on the retina without requiring the eye's lens to strain in order to compensate for an off-target focus.
How to Determine the Correct Prescription?
In clinical optometry, the goal is to measure the total refractive error and determine the MPMVA (Maximum Plus Maximum Visual Acuity)—the prescription that provides the best clarity at the minimum negative power (for myopia) or maximum positive power (for hyperopia) that still allows the patient to see 20/20 vision.
For myopia (negative prescription), the least minus power that achieves 20/20 vision is the correct prescription.
For hyperopia (positive prescription), the maximum plus power that achieves 20/20 vision is the correct prescription.
This is referred to as Full Correction.
Example:
If a patient’s actual prescription is -2.00D, their MPMVA is also -2.00D, which allows them to see 20/20.
- If the prescription given is less than -2.00D, the patient will have reduced visual clarity.
- If the prescription given is more than -2.00D (e.g., -2.25D, -2.50D, -2.75D, etc.), although the patient may still see clearly, it does not enhance vision but rather over-minuses the prescription.
The Myth of "Extra Clarity"
Over-minusing (providing a prescription stronger than necessary) does not actually improve clarity. Instead, it makes the image appear darker and smaller without increasing resolution. In fact, many patients with correct MPMVA can achieve vision even better than 20/20, often reaching 20/15+.
Thus, the idea that "seeing too clearly" exists is a myth—what actually occurs is over-minusing, which does not benefit vision but instead causes unnecessary strain and visual discomfort.
Hyperopia and MPMVA Principle
On the other hand, for patients who have congenital hyperopia (farsightedness) or a positive prescription, the MPMVA principle states that the highest plus power should still maintain clear vision equal to that of a normal person (20/20). The term"still maintain"is used because most farsighted individuals see clearly at a distance by relying on the eye’s accommodation (focusing ability). Therefore, we need to gradually reduce accommodation* by adding more plus power until reaching the highest plus value that still allows the patient to see clearly.
For example, a 30-year-old patient with good accommodation and congenital hyperopia of +2.00D will have an MPMVA of +2.00D. If we prescribe more than +2.00D, the patient will experience blurry vision at a distance. However, if we prescribe less than the actual hyperopia, such as +1.75D, +1.50D, +1.25D, +1.00D, or even0.00D (no correction at all), or a negative prescription, the patient may still see clearly but it would not be a full correction. Instead, it would be overminus or underplus, meaning the patient is seeing clearly by actively accommodating, which contradicts the correct definition of proper vision correction.
The further the prescription deviates from the actual refractive error, the less accurate the correction becomes. In Thailand, this is a common issue because patients with uncorrected hyperopia already see clearly with the naked eye, leading practitioners to hesitate in diagnosing the true refractive error out of fear that the patient will not see as clearly as before. As mentioned earlier, "marketplace vision tests focus only on clarity, not accuracy."
Overminus and Underplus in Automated Refraction
Overminus and underplus prescriptions are common when using automated refraction systems. This is because 99% of auto-refractor tend to overminus or underplus the prescription. The degree of error depends on the quality of the machine, which can range from low-quality Chinese models to high-end German devices. However, despite the quality variations, all auto-refractors inherently overminus to some extent.
Therefore, blindly trusting auto-refractors as a definitive diagnostic tool is highly concerning**. Seeing advertisements claiming"the most precise eye measurement"using auto-refractors is quite alarming.
Clarity Does Not Equal Accuracy
From the two previous examples, it is clear thatsharp vision alone does not indicate accuracy. Clarity does not determine whether a prescription is correct or incorrect because there are two types of clear vision:
1. Clarity with accommodation
2. Clarity without accommodation
For a prescription to be correct, the patient must see clearly without using accommodation, meaning the prescribed power should be the MPMVA as explained earlier.

Best Visual Acuity (BVA) and Balancing Both Eyes
The goal of MPMVA is to extract the full refractive error of each eye individually while ensuring the relaxation of accommodation. In clinical practice, from my tens years of experience, 95% of cases have different prescriptions between the two eyes. This means that if your test results show the exact same prescription in both eyes, you are likely part of the 5% minority of the population (but is that really the case?).
Because of this, off-the-shelf reading glasses can never be fully corrected for an individual's eyes. Furthermore, they are manufactured without considering the optical center alignment. These glasses are pre-made and sold without accounting for individual variations, making them highly unreliable. Choosing glasses by simply trying them on until you find one that “looks clear” is extremely risky. Many vendors unknowingly contribute to vision problems because they lack knowledge of the dangers associated with improper correction.
Once the MPMVA of each eye has been determined, the next step is to*balance both eyes to ensure they have equal clarity and function. This is called Best Visual Acuity (BVA), which involves binocular vision (whereas MPMVA only deals with monocular vision).
To achieve binocular balance, the focal points of both eyes must be equally positioned on the retina. This ensures that when the patient looks at objects at different distances, both eyes accommodate equally, preventing visual stress and discomfort.
The Importance of Balanced Vision
The visual nervous system functions as a unified system, meaning that vergence and accommodation always work together. The eyes cannot accommodate independently—they must function as a pair.
In other words:
Even if both eyes see clearly individually, it does not mean they are balanced
If one eye accommodates differently from the other, it can cause discomfort and dysfunction
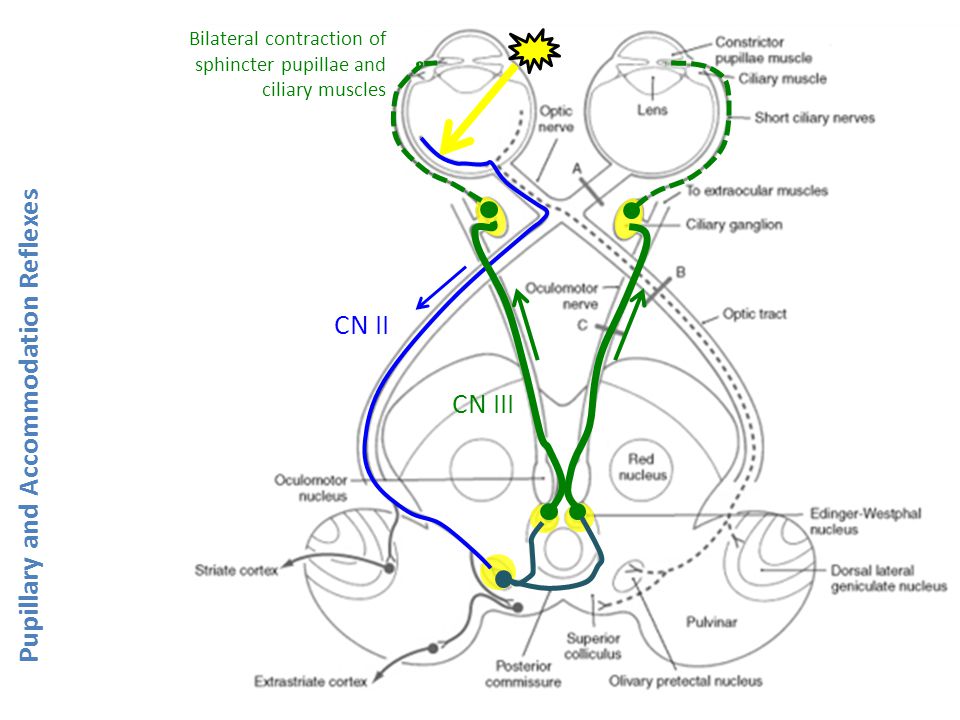
This diagram illustrates the pathway of the autonomic nervous system, showing the relationship between accommodation (focusing), pupil response, and convergence—all of which work together.
When one eye is stimulated, both eyes automatically respond simultaneously, a process often described as "input 1, output 2."
For example, if one eye focuses at one level and the other at a different level, they may seem clear separately, but not when used together. The brain cannot accommodate each eye independently, so this imbalance can cause*visual stress, headaches, or difficulty with binocular tasks like reading and depth perception.
Thus, after achieving binocular balance, the final step is to perform fogging/unfogging tests to ensure that both eyes focus perfectly on the retina without needing accommodation. This final B
Challenges of MPMVA Testing
Despite its accuracy, MPMVA is a subjective test, meaning it relies on patient responses. The biggest challenge is asking the right questions to ensure the patient understands and answers correctly.

This is an example of a subjective eye examination, where the patient's cooperation in responding to the examiner's questions is essential. This ensures that the results are both accurate according to clinical principles and satisfactory for the patient.
Miscommunication during the test can lead to incorrect prescriptions. Many patients struggle when asked "Which is clearer: 1 or 2?", and choosing incorrectly can result in an inaccurate prescription. If a patient adapts to an incorrect prescription over time, their visual function can deteriorate, which is a serious concern.
The Role of Experience and Knowledge in Subjective Testing
To perform subjective refraction accurately, the knowledge and experience of the examiner are critical as well as the patient’s physical and cognitive readiness.
Experience without knowledge results in stubbornness, where the practitioner blindly trusts their intuition without understanding the science behind their actions.
Knowledge without experience leads to rigidity, where the examiner struggles to adapt when faced with cases that don’t fit textbook scenarios.
Therefore, true expertise (Know-How) = Knowledge + Experience. This cannot be copied or bought.
Knowledge comes from formal education (universities) and self-study, requiring time, effort, and financial investment.
Experience comes from handling real cases, with complexity increasing over time, commonly referred to as "flight hours."
The Limitations of Auto-Refractors
Achieving true Know-How is not as simple as purchasing an auto-refractor with flashy advertisements claiming "the most precise measurement”.
Auto-refractors are not diagnostic tools; they are screening tools to provide an initial estimate.
Even a high-precision auto-refractor that measures to 0.1D still lacks accuracy and reliability for final prescription determination.
Thus, relying solely on computerized refraction is a serious mistake, often exploited in commercial markets that prioritize sales over proper vision care.
Final Thoughts
Achieving proper vision correction is not just about clarity but accuracy. A correct prescription should allow clear vision without forcing the eyes to accommodate. Understanding MPMVA, BVA, and binocular balance is crucial to ensuring both visual comfort and long-term eye health.
How to Obtain the Best Vision Prescription
The term "best" is inherently relative; it depends on specific factors, contexts, and comparisons at a given time. What was once considered the best may no longer be so. For example, the iPhone 4 was once the best Apple device, but today, the iPhone 16 Max Plus holds that title. The concept of "best" is always influenced by multiple factors and is relative to what we know at that moment. A frog living in a small well may believe its world is vast, just as a fish in a small pond may think its home is the largest body of water. When people lack knowledge, they often proclaim what they know as the ultimate truth. However, those with wisdom recognize that "the best" is often just marketing, and most advertising claims are not entirely true.
Determining the Most Accurate Vision Prescription
To measure the best (or most accurate) prescription at any given moment, we must first acknowledge that the human eye is a dynamic system controlled by the*autonomic nervous system. The crystalline lens inside the eye constantly adjusts its focus through the process of accommodation, either tightening or relaxing to change focus. Because of this constant adjustment, finding the true refractive error of the eye is challenging.
The key to an accurate eye exam is to temporarily convert the dynamic nature of the eye into a static state. This ensures that the prescription measured at that moment is as accurate as possible. The goal is to measure the relaxed state of accommodation. There are several methods to achieve this, ranging from pharmacological interventions to environmental adjustments:
1. Cycloplegic Refraction
This method involves using eye drops to temporarily paralyze the muscles responsible for focusing, a process called cycloplegia. It is particularly useful for children, whose natural focusing ability is strong. Without cycloplegia, a child's eye may stay in a state of excessive accommodation, leading to Pseudo-(false) myopia or incorrect measurements of hyperopia. In some cases, children with uncorrected hyperopia may develop strabismus (crossed eyes), amblyopia (lazy eye), or hidden strabismus. Cycloplegic refraction ensures the most accurate prescription by eliminating any residual focusing effort.
2. Infinity Distance Testing
The ideal testing distance for measuring relaxed accommodation is infinity. In practical terms, this means a testing distance of at least 6 meters (20 feet). An eye examination room should be designed to simulate infinity, allowing the patient to focus on a distant target naturally.
If the testing room is not at least 6 meters deep, the prescription obtained may be inaccurate because the eye will still be in an active focusing state. If a 6-meter testing distance is not available, a mirror-based optical system can be used to create an optical infinity environment. However, using shortened testing distances (such as near charts) is unacceptable because it fails to account for accommodation and convergence effects.
When a person looks at a distant object, their eyes are positioned straight ahead (primary gaze). However, when viewing a near object, the eyes must converge inward. This convergence triggers accommodation, making the measured prescription inaccurate. For this reason, measurements taken at distances shorter than 6 meters should not be considered clinically valid. Once the eye is in its most relaxed state—with accommodation fully released and the eyes in primary gaze—the next step is fogging.
3. Fogging
Fogging involves placing a plus-powered lens in front of the eye to shift the focal point in front of the retina, forcing the eye to relax its accommodation.
Even when testing at a 6-meter distance, some people—particularly latent hyperopes—may still be involuntarily accommodating. For example, a person with a true +2.00D hyperopia may still be exerting +2.00D of accommodation when looking far away. Without fogging, their eye may appear to have no refractive error (0.00D), leading to an incorrect prescription.
Fogging ensures that the accommodation system is truly relaxed, allowing for more accurate refraction. In subjective refraction, fogging is critical*for obtaining the best vision correction, particularly when determining: MPMVA (Maximum Plus to Maximum Visual Acuity
BVA (Best Visual Acuity)
Why "Best Vision Acuity" (BVA) Can Be Misleading
The best vision acuity (BVA) is determined by a combination of:
Sphere (Sph) – the main power of the lens
Cylinder (Cyl) – the correction for astigmatism
Axis – the orientation of the astigmatism correction
However, sphere and cylinder values can mask each other. This means that if the sphere is incorrect, the actual prescription may remain undetected, leading to false clarity.
Example: The Illusion of 20/20 Vision
A patient with the following prescription:
+1.00 DS / -2.00 DC
may still achieve 20/20 visionwithout correction because their spherical equivalent (SE) is calculated as:
SE = Sphere +Cylinder/2
SE = (+1.00) +(-2.00/2)= +1.00 + (-1.00) = 0.00
Since the spherical equivalent is 0.00, the patient may appear to have perfect vision (20/20), even though they have uncorrected astigmatism.
This is why visual acuity alone is not a reliable indicator of correct prescription. Many people with uncorrected astigmatism experience headaches, eye strain, fatigue, or nausea, despite achieving 20/20 vision. It is like seeing a clean room without realizing the dirt has been swept under the carpet.
The Importance of Determining the "Best Sphere"
The best sphere must be identified before measuring astigmatism. If the sphere value is incorrect, then the cylinder power and axis will also be incorrect, leading to misdiagnosis.
For example, if we assume a patient’s best sphere is 0.00 when it should actually be +1.00, we will fail to detect their -2.00 DC astigmatism. This is a common mistake in vision testing.
Conclusion
To obtain the most accurate prescription:
Use Cycloplegic Refraction for children and patients with strong accommodation.
Perform refraction at a 6-meter distance or use an optical infinity system.
Use fogging techniques to fully relax accommodation.
Do not rely solely on 20/20 visual acuity—it does not guarantee an accurate prescription.
Carefully determine the best sphere before measuring astigmatism.
By following these principles, we can ensure that the prescription obtained is as accurate and comfortable as possible, reducing unnecessary eye strain and visual discomfort.
Where is the Best Sphere?
The best sphere is the optimal spherical value before determining the cylindrical correction. It may be in the form of an actual best sphere or a spherical equivalent, which is essential for further calculations.
How to Find the Best Sphere
There are multiple methods to determine the best sphere, but relying on the sphere value measured by an autorefractor can be risky. What happens if the machine measures 0.00 or a negative value when the actual prescription should be Sph +1.00DS and Cyl -2.00DC? Many hyperopic children end up wearing minus lenses just because the autorefractor misclassifies their vision, sometimes leading to visual dysfunction or even strabismus. Whether due to ignorance or oversight, the consequences remain.
Based on over 15 years of optometric experience, the most reliable method is retinoscopy, an objective test that provides accurate readings in over 90% of cases (personally, I believe it exceeds 98% compared to an autorefractor).
- Hyperopia: Light moves with movement
- Myopia: Light moves against movement
- Astigmatism: Light moves in a circular or scissor motion
- Emmetropia: look bright light with no movement
Retinoscopy is not influenced by the examiner's vision, unlike subjective refraction. Whether the examiner wears glasses or not, their accommodation does not affect the patient's results. The only limitation is whether the examiner can clearly see the light reflex.
Objective vs. Subjective Testing
While retinoscopy (objective test) and subjective refraction (subjective test)may yield slightly different results, retinoscopy provides the foundation, and subjective refinement polishes the prescription. Skipping objective testing is like polishing an unshaped rock—it won’t result in a useful final product.
Retinoscopy with Fogging
One major advantage of retinoscopy is the ability to check the focus of light at infinity, something autorefractors cannot accurately simulate.
- Over-refraction can help detect an over-minused prescription
- A proper fogging lens should maintain VA at 20/100, not completely blur the vision
- Insufficient fogging leads to pseudo-myopia, while excessive fogging forces accommodation
Alternative Methods for Determining Best Sphere
1. Red/Green Test
- The point where both red and green are equally clear can guide best sphere determination.
- However, subjective factors such as perception, color vision, and lens opacity can cause errors.
2. Fog & Clock Chart
- If retinoscopy doesn’t reveal astigmatism, a clock chart can be used under mild fogging (VA 20/30) to check for astigmatism.
- The Clock Dial Test can estimate cylinder power and axis before refining with aJackson Cross Cylinder (JCC) test.
Dangerous Misconceptions
A concerning question I once received:
"Can we fog until blurry, then unfog until blurry again, and use the midpoint as the prescription?"
This fire-element thinking is fundamentally flawed. For example, a 5-year-old child with true plano vision (0.00D) may fog at +1.00D but require -10.00D to make 20/40 letters blurry again due to strong accommodation. Would you prescribe -5.50D? Clearly not!
This misunderstanding of anatomy and physiology is akin to using herbal eye drops, bamboo thorns for cataract treat , or unscientific treatments—misguided practices based on ignorance.
The Right Prescription vs. The Preferred Prescription
Best Visual Acuity (BVA) is both an art and a science. There is a difference between:
- The "right" prescription (what the eyes truly need)
- The "preferred" prescription (what the patient finds comfortable)
A final prescription should be determined only after obtaining the true refractive error, not before. If the true values aren’t established, any modifications are merely guesswork.
Ultimately, if the actual refractive error is properly identified, the "right" and "preferred" prescriptions should be the same, just as no one would choose shoes that don’t fit. Altering the prescription without a valid reason is often due to not knowing the real values in the first place.
Final Thoughts
Eye examination is a delicate process, yet it is unfortunate that in our country (third world Thailand), vision care is often seen as merely a means to sell glasses. If we look at it objectively, when we think of the eyewear business, what comes to mind first? Promotions, discounts, giveaways—rather than the clinical aspect, which should be the core and most important part of the service. Eye exams are frequently reduced to a marketing tool—offered for free to encourage eyewear sales—rather than being valued as a crucial step in ensuring accurate vision correction. Worse still, there are no clear regulations governing the standards of eye examinations.
Unlike other industries where discounts are based on outdated models or stock clearance (e.g., cars, smartphones, computers, food products), the eyewear industry often applies discounts even on newly released products. This practice stems from habitual markup and discounting, which has shaped how eyewear businesses operate—prioritizing pricing tactics over professional standards.
If we abandon the standards of eye examinations, then no matter how much innovation or advanced technology scientists develop to improve vision quality, it will be in vain. Millions of prescription lenses are manufactured each year, but how many people actually receive lenses that truly match their needs?
The root cause is the lack of a universal standard for vision care—without clear guidelines on what constitutes a proper eye exam, inconsistent and subpar practices will continue to emerge unchecked. This will remain an ongoing issue without an end in sight.
Sometimes, we just have to accept the reality and move forward.
Thanks for your reading till end , I hope you will accept compromise part of eye care in Thailand and built it better and better.
See you next.
Dr.Loft ,O.D.

578 Wacharapol rd, Tharang ,Bangkhen ,BKK 10220
mobile : 090-553-6554
www.facebook.com/loftoptometry
lineid: loftoptometry
www.loftoptometry.com
